Surgery. Making all the machines talk to each other.
Twenty-eight-year-old Andrew was being prepped for hand surgery due to an injury.
Alert and curious, Andrew was greeted by what seemed like a dozen health professionals coming and going, all introducing themselves, asking questions, listening to his answers and explaining in detail what was about to happen.
He even joked a little throughout the prelude to anesthesia oblivion.
The last thing on his mind was the sophisticated medical device integration his surgical team would rely on.
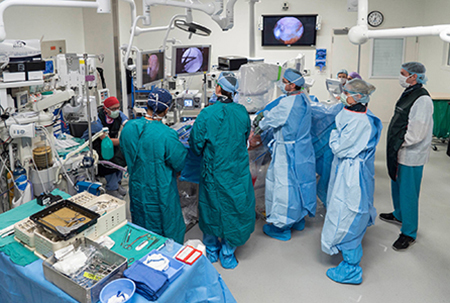
Some of our projects have high visibility, like Epic. And some seem to happen behind the scenes with little fanfare. The recent medical device integration is one example of a high-impact clinical technology for patients in acute care settings.
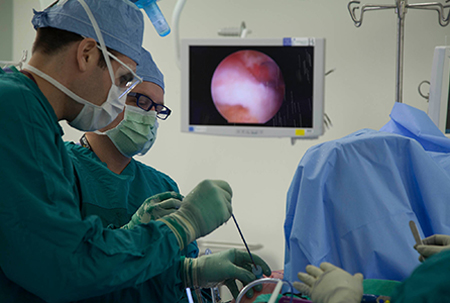
Less time with machines. More time with patients.
Hospital care requires a lot of technology functioning in concert.
Juggling all the information pouring in from disparate medical devices can be daunting for even the most skilled clinician. Especially when the prime directive is caring for the patient – not the machine.
These medical devices monitor things like a patient’s vital signs, as well as ventilator and anesthesia equipment. This patient data feeds directly into Epic.
The biggest gains come from reduced manual entry. This yields two major improvements – reducing the risk of data entry errors and freeing up clinical staff to spend more time with patients, because they spend less time keying in data.
In critical care settings like the ICU, the medical devices virtually plug into Epic, providing a continuous feed of patient data. In addition to vital signs, this can include data from devices like a patient’s ventilator, cardiac monitor, cerebral and tissue oximeter, hemodynamic monitor and brain monitor.
That’s a lot of patient information to keep track of, reinforcing the key benefits of medical device integration – better data because of less manual data entry.
Better patient care.
In the OR, an entire dashboard of data flows directly to the patient’s Epic record. One example of improved patient care – freeing up the anesthesiologist to focus on the patient, rather than enter the patient information by hand.
In the nursing arena, Capsule Chart Xpress ™ is a rolling vital sign station nurses push from room to room.
Capsule Chart Xpress simplifies everything. It makes it possible for a nurse to scan a patient’s armband to verify identification, collect vital signs and record other things like oxygen source, urine volume, pain scale and bed safety. Then simply review and confirm results – by pressing a ‘Send Vitals’ button. All that data then shows up in the patient’s Epic record.
“This makes it easier for care teams,” said Melita Howell, manager of medical device integration. “If this is broken, it’s more difficult for them. They used to write everything on paper, contributing to error, and it was a much slower process.” But not anymore.
Medical device integration contributes to better patient safety and care. So patients like Andrew can benefit from the technology, even when they never knew it was there.
